A 91-year-old patient of a nursing home was allowed to develop a pressure ulcer (bed sore, bedsore, pressure sore, decubitus ulcer) on her sacrum (low back). The pressure ulcer deteriorated and she died three and one-half months later.
On admission to the nursing home, the patient did not have any pressure ulcers. She was, however, dependent on the nursing home’s staff for turning and resposition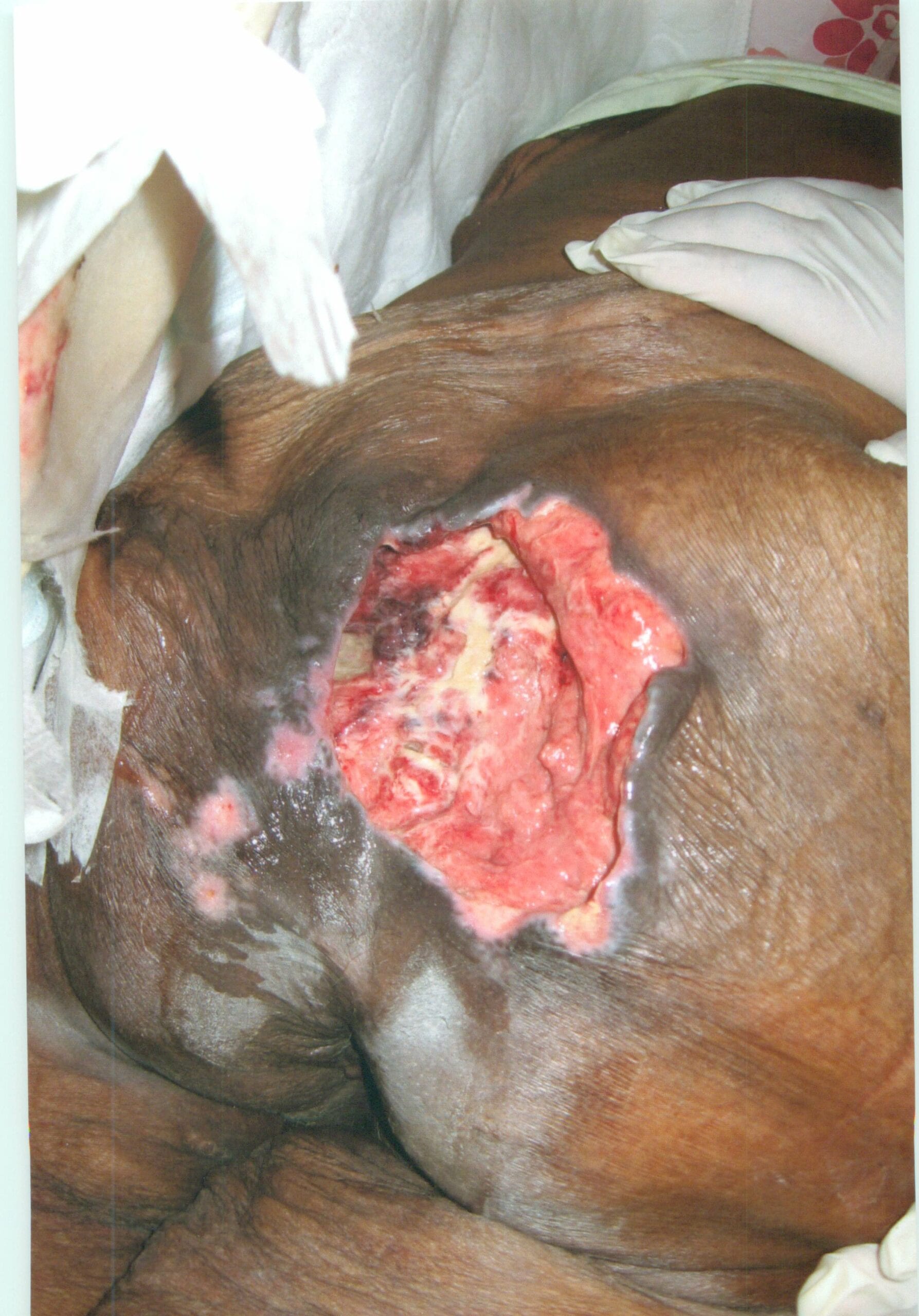
Within three weeks after the pressure ulcer (bed sore, bedsore, pressure sore, decubitus ulcer) was first observed, the wound was documented to have been “worsening, with more maceration seen on wound edges.” Several days later, the pressure ulcer was noted to have increased in size from 4.0 cm x 2.5 cm to 5.0 cm x 3.5 cm and 50% of the wound bed was documented to have been comprised of necrotic tissue.
The patient thereafter was admitted for one week to a local hospital for reasons unrelated to the wound. On admission to the hospital, the patient’s pressure ulcer (bed sore, bedsore, pressure sore, decubitus ulcer) was documented to be stage II with dimensions of 7 cm x 3 cm – a 20% increase in size in the three days before her hospital admission. When she was discharged from the hospital one week later and returned to the nursing home, the pressure ulcer (bed sore, bedsore, pressure sore, decubitus ulcer) was “unstageable” with dimensions of 5.0 cm x 6.2 cm and 80% dark brown slough. The nursing home claimed the hospital was to blame for the deterioration of the ulcer during the patient’s hospitalization. We contended the deteri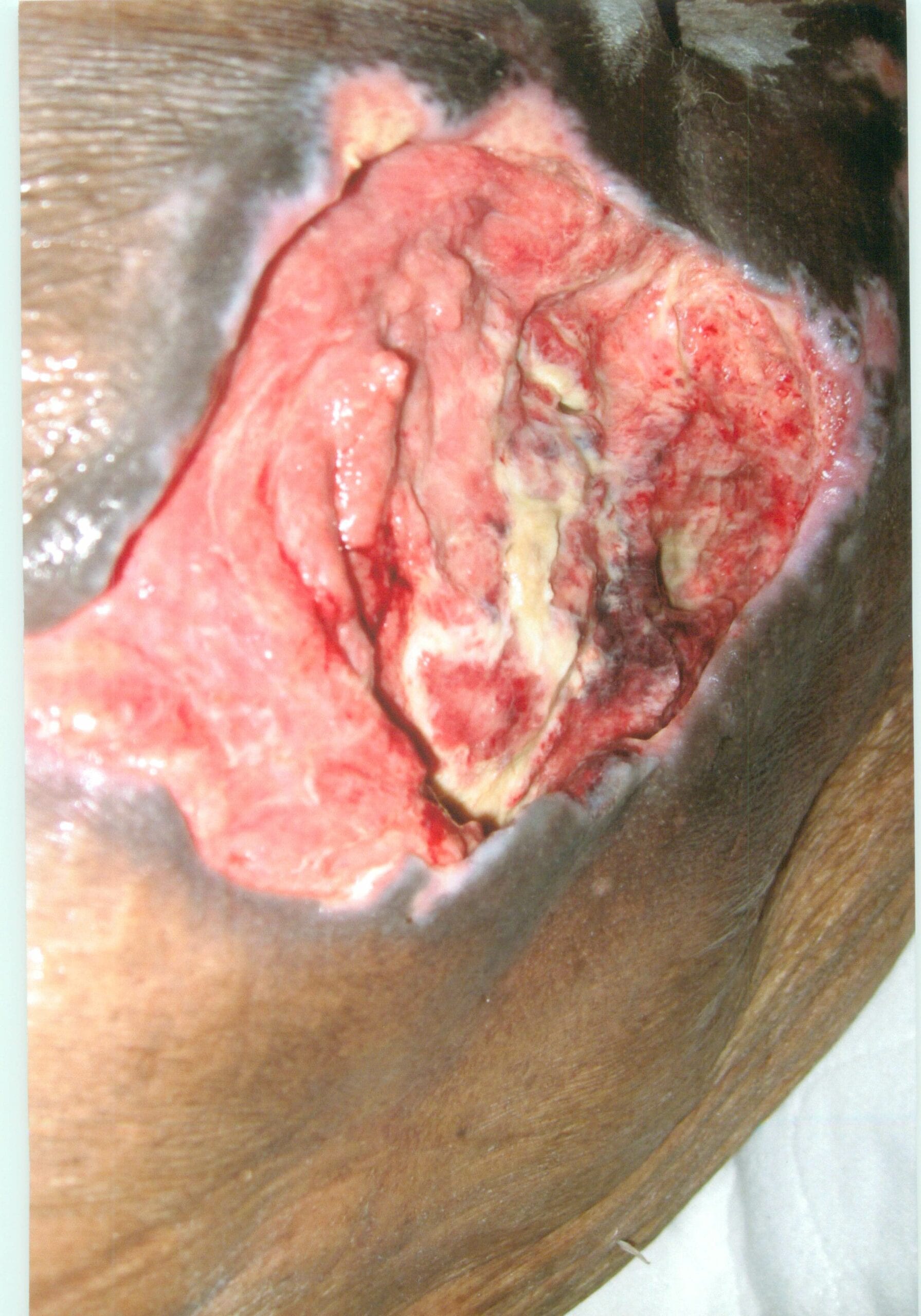
As the nursing home’s failures to turn and reposition the patient continued, the pressure ulcer continued to deteriorate. Within a couple of weeks after the patient’s hospitalization, and despite aggressive wound therapy, the wound measured 11.0 cm x 11.0 cm, had purulent drainage (pus), an odor, and was contaminated with MRSA. The patient was discharged from the nursing home to her own home with hospice care. Even though pain medication was prescribed for use at home, the patient frequently experienced “breakthrough pain” from the ulcer, especially before and after dressing changes and when repositioned. The patient died several weeks later as a direct result of sepsis (systemic infection) caused by the pressure ulcer (bed sore, bedsore, pressure sore, decubitus ulcer). She was survived by two daughters and a granddaughter.
The nursing home contended the patient’s pressure ulcer was unavoidable because of the patient’s age, poor nutritional status, and chronic end stage kidney disease. Her kidney disease prevented her from eliminating waste products and fluid from her blood. She had pre-existing hypoalbuminemia (low protein), which typically would have required her protein level to be supplemented. However, if she had received additional protein, an even greater buildup of protein would have occurred because of the kidney disease and kidney failure would have resulted. The nursing home also contended that, despite the family’s claims, the patient was consistently and timely turned and repositioned
The case settled for $400,000 well before trial.
________________________________________________________________
Robert W. Carter, Jr. is a Virginia attorney whose law practice is dedicated to protecting the rights of the victims of nursing home and assisted living neglect and abuse in Richmond, Roanoke, Norfolk, Lynchburg, Danville, Charlottesville, and across Virginia

